Common Foot Problems
Common Foot Problems: do you have these ailments?
Many people believe that it is natural for their feet to hurt. That isn’t true. Any time you have foot pain that lasts longer than a week you should get the pain examined by a qualified foot specialist, these include the following:
Family Doctor
Podiatrist
Chiropodist
Pedorthists
Orthotists
Chiropractor
Allied Health Care Practitioners
Some common foot conditions in which the application of Custom Foot Orthotics is beneficial are listed below:
Flat Feet
PES PLANUS; aka FLAT FEET, the PRONATED FOOT:
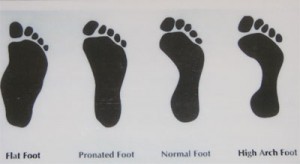 Low arched, or flat feet, are a common type of foot structure.
Low arched, or flat feet, are a common type of foot structure.
Most flat feet are pronated which is a foot in poor functional position. Close examination of this type of foot in a weight-bearing position shows:
- turning out of the heel bone away from the centre of the body
- inward rotation of the leg
- bulging of the inner aspect of the ankle
- shifting of the forefoot outward from the heel
Orthotic Management:
Treatment starts with a proper evaluation of the underlying cause of the conditions to diagnose the appropriate correction.
Functional Custom Foot Orthotics to compensate for mechanical faults, will allow your feet to function with improved efficiency. Orthotics relieve stress from compromised joints, ligaments and muscles, diminishing deforming forces acting on the foot.
Heel Pain
HEEL PAIN, PLANTAR FASCIITIS, AND BONE SPURS:
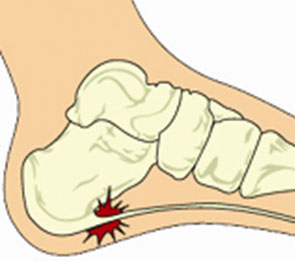 Sharp pain, aching or stiffness on the bottom of one or both heels is a very common ailment.
Sharp pain, aching or stiffness on the bottom of one or both heels is a very common ailment.
Pain from Plantar Fasciitis is often at its worst upon awakening in the morning (or after sitting down for an extended period and then resuming activity). This pain causes hobbling or a limping gait pattern for a few minutes before a comfortable stride can be resumed.
As weight continues to be applied during walking or standing, mild or severe pain may persist.
Another cause of heel pain is bone spurs, where bone growth originates from the heel bone (Calcaneous) and pinches into the tendons of the heel from the Achilles tendon.
Injury, overuse, loss of fat pad and/or non-presence of fat tissue on the heel can also cause heel pain.
Orthotic Management:
Padding added to the dorsal surface of the orthotic will aid in comforting the heel bone; the addition of soft heel spur pads will help to support the perimeter of the heel bone to aid in pain management and healing time. Addition of a hole in the shell material of the orthotic with a soft orthopaedic material plug will aid in decreasing forces on the central axis of the heel. The main support of an orthotic will help maintain proper heel bone alignment to balance the forces acting on the tissues and muscle of the foot to prevent overuse, inflammation and injury.
Bunions
BUNIONS (HALLUX VALGUS):
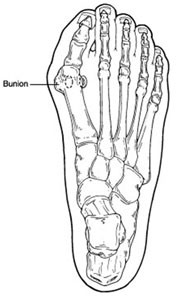 A common deformity of the big toe joint, a bunion occurs mostly in people who have flat feet or who wear tight fitting footwear that are too small for their dynamic foot size.
A common deformity of the big toe joint, a bunion occurs mostly in people who have flat feet or who wear tight fitting footwear that are too small for their dynamic foot size.
Women are more frequently affected with bunions because of tight, pointed, confining or high heeled shoes. Wearing high heels is especially stressful on the joints of the foot because all of the body’s weight rests on the ball of the foot; the foot is then forced into a narrow, pointed toe box, compounding the problem.
Older people are also vulnerable to bunions because of the higher incidence of arthritis affecting the big toe joint.
A bunion is a protuberance of bone or tissue around the joint. The enlargement occurs either at the base of the great toe or on the outside of the foot, at the base of the little toe. This is called a “bunionette” or “tailor’s bunion.”
Orthotic Management:
Custom Foot Orthotics help maintain proper foot alignment and function thus forcing the toes to be evenly placed on the ground during walking and running. This even placement will prevent the over use or misalignment of the first toe and prevent excessive forces acting on it’s joints and displacing the bones. The Custom Foot Orthotic will also support the arch of the flat foot preventing it from overpronating and reducing added forces on the big toe joint.
Several modifications to the orthotic will also aid in bunion treatment, these include: 1st metatarsal cut outs, 1st ray cut-outs, reverse Morton’s extensions and kinetic wedges.
Diabetes
DIABETES
Because diabetes is a systemic disease affecting many different parts of the body, ideal case management requires a team approach. The Podiatrist Physician, Pedorthist, Chiropodist, Chiropractor and Allied Health Professional are an integral part of the treatment team and work effectively in the prevention of amputations.
The key to amputation prevention in diabetic patients is early recognition and regular foot screenings, from a Podiatric Physician.
In addition to these check ups, there are warning signs that you should be aware of so that they may be identified and called to the attention of the family physician or podiatrist. They include:
- Skin color changes
- Elevation in skin temperature
- Swelling of the foot or ankle
- Pain in the legs
- Open sores on the feet that are slow to heal
- Ingrown and fungal toenails
- Bleeding corns and calluses
- Dry cracks in the skin, especially around the heel
Wound Healing:
Ulceration is a common occurrence with the diabetic foot, and should be carefully treated and monitored by a Podiatrist to avoid amputations.
Poorly fitted shoes, or something as trivial as a stocking seam, can create a wound that may not be felt by someone whose skin sensation is diminished due to neuropathy. Left unattended, such ulcers can quickly become infected and lead to more serious consequences.
Your Podiatric Physician knows how to treat and prevent these wounds and can be an important factor in keeping your feet healthy and strong. New to the science of wound healing are remarkable products that have the appearance and handling characteristics of human skin. These living, skin-like products are applied to wounds that are properly prepared by the Podiatric Physician. Clinical trials have shown impressive success rates.
If You Have Diabetes Already . . . DO:
Wash feet daily
Using mild soap and lukewarm water wash your feet in the mornings or before bed each evening. Dry carefully with a soft towel, especially between the toes, and dust your feet with talcum powder to wick away moisture. If the skin is dry, use a good moisturizing cream daily, but avoid getting it between the toes.
Inspect feet and toes daily
Check your feet every day for cuts, bruises, sores or changes to the toenails, such as thickening or discoloration. If age or other factors hamper self-inspection, ask someone to help you, or use a mirror.
Lose weight
People with diabetes are commonly overweight, which nearly doubles the risk of complications.
Wear thick, soft socks
Socks made of an acrylic blend are well suited, but avoid mended socks or those with seams, which could rub to cause blisters or other skin injuries.
Stop smoking
Tobacco can contribute to circulatory problems, which can be especially troublesome in patients with diabetes.
Cut toenails straight across
Never cut into the corners, or taper, which could trigger an ingrown toenail. Use an emery board to gently file away sharp corners or snags. If your nails are hard to trim, ask your podiatrist for assistance.
Exercise
As a means to keep weight down and improve circulation, walking is one of the best all-around exercises for the diabetic patient. Walking is also an excellent conditioner for your feet. Be sure to wear appropriate athletic shoes when exercising. Ask your podiatric physician what’s best for you.
See your podiatric physician
Regular checkups by your podiatric physician are the best way to ensure that your feet remain healthy.
Be properly measured and fitted every time you buy new shoes
Shoes are of supreme importance to diabetes sufferers because poorly fitted shoes are involved in as many as half of the problems that lead to amputations. Because foot size and shape may change over time, everyone should have their feet measured by an experienced shoe fitter whenever they buy a new pair of shoes.
New shoes should be comfortable at the time they’re purchased and should not require a “break-in” period, though it’s a good idea to wear them for short periods of time at first. Shoes should have leather or canvas uppers, fit both the length and width of the foot, leave room for toes to wiggle freely, and be cushioned and sturdy.
Don’t go barefoot
Not even in your own home. Barefoot walking outside is particularly dangerous because of the possibility of cuts, falls and infection. When at home, wear slippers. Never go barefoot.
Don’t wear high heels, sandals, or shoes with pointed toes
These types of footwear can put undue pressure on parts of the foot and contribute to bone and joint disorders, as well as diabetic ulcers. In addition, open-toed shoes and sandals with straps between the first two toes should also be avoided.
Don’t drink in excess
Alcohol can contribute to neuropathy (nerve damage) which is one of the consequences of diabetes. Drinking can speed up the damage associated with the disease, deaden more nerves and increase the possibility of overlooking a seemingly minor cut or injury.
Don’t wear anything that is too tight around the legs
Panty hose, panty girdles, thigh-highs or knee-highs can constrict circulation to your legs and feet. So can men’s dress socks if the elastic is too tight.
Never try to remove calluses, corns or warts by yourself
Commercial, over-the-counter preparations that remove warts or corns should be avoided because they can burn the skin and cause irreplaceable damage to the foot of a diabetic sufferer. Never try to cut calluses with a razor blade or any other instrument because the risk of cutting yourself is too high, and such wounds can often lead to more serious ulcers and lacerations. See your podiatric physician for assistance in these cases.
Your podiatrist physician/surgeon has undergone extensive training in the diagnosis and treatment of all manners of foot conditions. This training encompasses all of the intricately-related systems and structures of the foot and lower leg including neurological, circulatory, skin and the musculoskeletal system, which includes bones, joints, ligaments, tendons, muscles and nerves.
– Information courtesy of The American Podiatric Medical Association
Orthotic Management:
The application of a soft or accommodative Custom Foot Orthotic constructed from a non corrected positive of your foot will aid in maintaining healthy feet.
The fabricated orthotic device will decrease shear forces acting on the tissue of your feet while dispersing ground reaction and gravitation forces on your feet.
The special material in our Diabetic Orthotic allows the device to be soft and flexible while maintaining its shape over time and not breaking down like several other non-custom diabetic Orthotics.
Achilles Tendonitis
ACHILLES TENDONITIS:
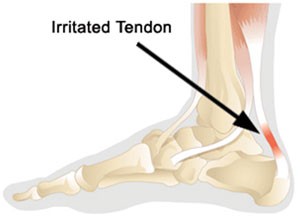 Achilles Tendonitis is characterized by inflammation of the sheath surrounding the Achilles tendon.
Achilles Tendonitis is characterized by inflammation of the sheath surrounding the Achilles tendon.
The presence of pain behind the heel, ankle and lower calf are signs of this condition.
The condition arises from counter rotational forces acting on the tibia against the femur as a result of excessive pronation of the feet which causes the heads of the tendon to torque against one another and over stretch the tendon.
Orthotic Management:
Custom Foot Orthotics help maintain function and alignment of the heel and prevent over pronation of the foot.
Additions of rear foot posts to stabilize the orthotic device inside your footwear with a removeable heel lift of about 3mm or 1/8 inch will allow the Achilles tendon to be lax and not stretched while in its resting state. The application of the heel lift is only temporary, for about 6-8 weeks until further consultation by your foot specialist’s follow-up assessment.
Ball of the Foot Pain
METATARSALGIA, a.k.a Ball of the foot pain:
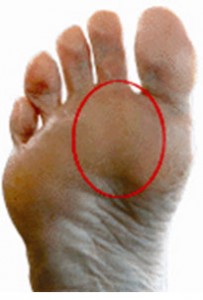 Metatarsalgia is a general term used to denote a painful foot condition in the metatarsal region of the foot (the area just before the toes, more commonly referred to as the ball-of-the-foot).
Metatarsalgia is a general term used to denote a painful foot condition in the metatarsal region of the foot (the area just before the toes, more commonly referred to as the ball-of-the-foot).
This is a common foot disorder that can affect the bones and joints at the ball-of-the-foot.
The first step in treating metatarsalgia is to determine the cause of the pain.
If improper fitting footwear is the cause of the pain, the footwear must be changed. Footwear designed with a high, wide toe box (toe area) and a rocker sole is ideal for treating metatarsalgia. The high, wide toe box allows the foot to spread out while the rocker sole reduces stress on the ball-of-the-foot.
Orthotic Management:
Custom Foot Orthotics designed to relieve ball-of-foot pain usually feature a metatarsal pad.
The Custom Foot Orthotic is constructed with the pad placed behind the ball-of-the-foot to relieve pressure and redistribute weight from the painful area to more tolerant areas. Other products often recommended include gel metatarsal cushions and metatarsal bandages. When these products are used with proper footwear, you should experience significant relief.
Service
We back our product and offer excellent support for fitting and adjusting.
Quality
Custom made orthotics that last! Your customers will be impressed.
Care
Our customers are the backbone of our business. We make sure you are cared for.

